
In the Adivasi settlements around Maharashtra’s Melghat tiger reserve, dais like Ropi and Charku have for decades handled home deliveries. But both are elderly and there is no one to carry forward their legacy.
There are two babies in there, Ropi told the doctor at the private maternity clinic, confidently – though she didn’t have any ultrasound report to refer to.
Ropi Mannu Bete recounts the incident from around two years ago with some relish and much mirth. “Kaan me woh lagaya [She wore that thing in her ears],” she says, miming the doctor using a stethoscope. The doctor took a final look at the frail pregnant woman’s moderately sized belly and disagreed with Ropi’s forecast of twins.
“Medam, do hota, do [Two madam, there will be two],” she repeated, before backing off to sit on a stool in the delivery room of the clinic. The 70-something Ropi and the mother-to-be, writhing in pain by then, were in Paratwada town, 20 kilometres from Jaitadehi, their village on the fringes of the Melghat forest in northeastern Maharashtra.
By evening, a boy was born and, seconds later, a second baby’s head emerged. A girl this time, a twin sister.
Ropi laughs loudly, seated on a bare wooden cot at one end of the verandah of her traditional mud-wall house, its floors swabbed to a sheen with cow dung. Inside, the three rooms with wooden rafters are empty, her grown-up sons away at work on the two acres the family cultivates.
She lets out an expletive in Korku – literally translated as a donkey’s privates – and laughs some more, the lines etched on her face deepening. “That’s what I told her,” she says, a little smug at the memory of hurling an abuse at a city doctor.

Ropi, Jaitadehi village’s last remaining traditional dai , says she must have delivered at least 500-600 babies
That confidence comes from more than four decades of experience. Ropi, who belongs to the Korku community, is Jaitadehi’s last remaining traditional dai, and says she must have delivered at least 500-600 babies. She never kept count. Not a single still-birth occurred when she was in charge of delivery, she says, with evident pride. “ Sab chokha [They were all fine].” Dais are traditional birth attendants (TBAs) who serve as midwives, though they don’t have any modern training or certification.
For the Korku tribals of the Melghat forest, living in the villages of Dharni and Chikhaldara blocks of Amravati district in Maharashtra’s Vidarbha region, women such as Ropi have long been more than just keepers of a tradition to birth babies at home. As experienced midwives, they also provide ante-natal care and provide health service in remote, forested and hilly areas from where rapid movement out for medical purposes is often not possible.
Most villages in Melghat still have one or two dais, but they are all elderly now, says Ropi, and the next generation of TBAs has not emerged. Jaitadehi’s only other dai died several years ago. Ropi reckons that she may have left behind a daughter or a daughter-in-law who picked up the skills, but nobody from that family has since worked as a dai.
Ropi’s own children were all born at home, assisted by her mother and a dai. She had four sons, one of them died of illness over a decade ago. She also has two daughters, both married and living in Jaitadehi itself, and a bunch of grandchildren and great-grandchildren. (Her daughters have refused to take up this work, though one daughter did learn the skills a little, Ropi says.)
“My daughter-in-law gets so scared, she won’t even stand with me in the room where a woman is giving birth,” she adds. “She won’t watch or hand me the sutures or cloth or anything. Aisa kaapne lagta [She begins to shiver],” she says, mimicking the younger woman’s shudder at the sight of blood.
Older generations of women didn’t fear bodily functions, Ropi recalls. “We didn’t have a choice, we had to be brave. There were no doctors and nurses to run to for every small thing.”
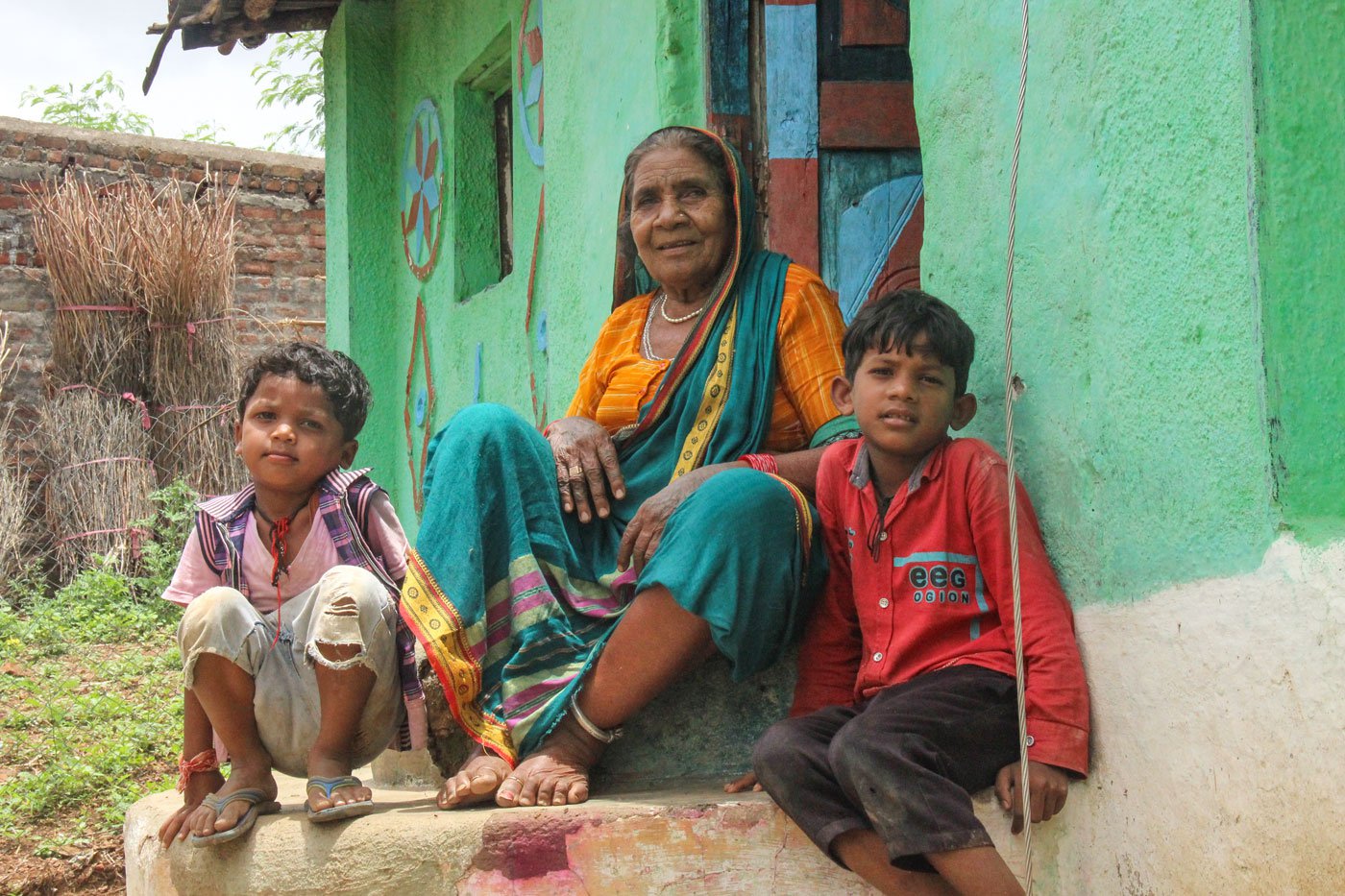
Ropi with her great grandchildren: her own children were all born at home, assisted by her mother and a dai
Her mother and grandmother were both dais , and she learned the skills while accompanying her grandmother on the job. Ropi says her mother wouldn’t let the restive daughter – who never went to school – go along when she visited homes to deliver babies. “ Bakei hejedo [Stay back],” she would scold the young girl in Korku, she remembers. “But my granny would take me along, even when I was only 12 or 13.” So even before she got married at around the age of 16, Ropi had begun to work as her grandmother’s assistant.
*****
The rolling hills and forests of Melghat – a major biodiversity repository – are home to the vast Melghat Tiger Reserve, spread across more than 1,500 square kilometres. The dry, deciduous forest has villages that are home to Korku and Gond indigenous communities. Many of these Adivasi settlements are located inside the tiger reserve, in its buffer area and on the fringes. The people here are mostly farmers and pastoralists and also depend on forest produce such as bamboo and herbs as sources of income.
Bortyakheda, a hamlet of 150 families in the core forest area, is located nearly 50 kilometres from the taluka town of Chikhaldara. Here, Charku Babulal Kasdekar, around 70 years old, has been a dai for “as long as I can remember.” She says even today in Melghat’s remote villages, of every 10 pregnant women, the families of about five prefer to home-birth a baby, though access to medical facilities has improved a little over the decades. (The 2015-16 National Family Health Survey, NFHS-4 , notes that over 91 per cent births in rural areas were institutional deliveries, a number that may not cover the specific realities of remote villages in Melghat).
In April 2021, Bortyakheda got a sub-centre of a primary health centre (PHC), a single-storey structure that was still to get piped water two months later, when I visited. There is an auxiliary nurse-midwife (ANM) on call here, available 24 hours. She’s supposed to live in a residential space on the first floor, but Bortyakheda’s ANM, Shanta Vihike Durve, is a local, married into the village.
The sub-centre has a post for a doctor to serve as the designated community health officer, but the absence of piped water is a deterrent for anybody appointed to the post, villagers told me. A newly graduated doctor, who was undergoing training at the PHC in Semadoh village, around 20 kilometres away, was expected to join soon (around the time I visited last year).

Bortyakheda’s ANM Shanta Durve (left) urges Charku, the village’s elderly dai, to come along even for deliveries the PHC
But many pregnant women prefer to not visit the sub-centre, says the ANM. “There is an element of trust in a woman from among their own overseeing their delivery,” adds Shanta, who is in her early 30s and posted here after a decade’s experience at the sub-centre in the adjacent Morshi block.
She urges Charku to come along even when deliveries are done at the PHC in Semadoh. Families are more amenable to accepting the dai ’s advice, says Shanta, and rues the fact that Bortyakheda no longer has any young dais , nobody who will carry forward Charku’s legacy of service. A second dai in the village has almost stopped working due to old age, and also didn’t undergo a short training course organised by the government along with UNICEF some years ago.
Charku, who participated in the day-long course, says, “We think we know everything, but they taught us some more important things, like how essential it is to use soap, how to wash our hands, and to use a new blade.”
In those instances when she accompanies a woman in labour to the PHC or, rarely, to a private clinic, the delivery is handled by a (female) nurse. The women, Charku says, will avoid a male doctor until the nurse says she cannot handle it. A doctor is summoned only if there is a complication.
Charku does not receive any payment for these visits. Why does she still go along? “ Chalo bola to jaati [I go if they ask me to]. Why should I not go if the mother is comforted by my being there?”
Years ago, Charku says, she would be paid in grain, two or three measures of rice or wheat – in a pai, a traditional brass vessel resembling a large tumbler. Sometimes there was a small cash bonus.
The dais’ earnings have not improved greatly over the decades. For Charku’s last delivery a week before I met her in June 2021, she was paid Rs. 500 and four kilos of wheat. It was a quick childbirth, the baby emerging almost as soon as labour pains began. “Even if it was a long labour, I’d have been paid the same amount,” she says.

Charku with two of her great-grandkids: at least half of the babies born in Bortyakheda over the past three decades had Charku present at the time of their birth, and she has delivered her own grandchildren and a great-grandchild
Charku’s husband died around five years ago; he used to till an acre of land which her daughter and son-in-law now cultivate. There was never a steady income from her work as a dai, Charku says. Some months in recent years she has earned up to Rs. 4,000, and some months not even Rs. 1,000.
At least half of the babies born in Bortyakheda over the past three decades had Charku present at the time of their birth, the women here estimate. Charku has delivered her own grandchildren and a great-grandchild.
Some newborns she delivered died a few days later, she recalls. “Not during the birth, but a few days later.” She doesn’t know the cause of these deaths. Nobody knows, she reasons.
Now, with her eyesight dimming, she finds herself telling families more and more frequently to head to the PHC or the new sub-centre.
*****
Ropi, who doesn’t know exactly how old she is, has been having trouble with her legs lately. There is swelling around the ankles and her knees hurt terribly. She hasn’t seen a city doctor about it, and rubbing the oil prescribed by a local vaid (an alternative medicine practitioner) has not helped.
Though she continues to roam around the village meeting old acquaintances and visiting her daughters, she has been refusing most of the families who approach her for deliveries, unsure if she can manage outside her home long enough and if her sight is good enough. “I tell them to call the city clinic [in Paratwada town], and I wait with them until the ambulance arrives. Sometimes I go along if the vehicle is going to return to the village immediately,” Ropi says.
Ropi’s family has a small goat-rearing business, and they also cultivate two acres. Her earning as a dai remain modest, and have not improved greatly over the decades
In the years when she was a busy dai , she was known in Jaitadehi for her quick and calm way of responding to situations. “Earlier, when they would come to call me, I would first tell them what all things I would need — a blade, dhaaga [thread, referring to sutures], sui [needle].” Many dais are adept at sewing up the perineal tear, she shrugs as if it is no big deal.
Then, depending on whether the labour had only just begun or was already advanced, she would finish her chores and walk briskly to the house of the mother-to-be, where anxious family members would be gathered.
Ropi always began with a prayer, then washed her hands before inspecting the dilation of the woman in labour.
“The mother [of the mother-to-be] doesn’t do anything, but she’s always at the side of her daughter, also wailing. The mother’s pleas would match her daughter’s cries in pain. ‘O maai, jaldi kar do maai’ , the mothers would call out [‘Oh mother, end her pain quickly, mother’]. As if that’s in my hands!” Ropi exclaims.
Sometimes labour pains would continue for hours and Ropi would return home to quickly grab a bite, or serve a meal to her husband or a son. “In those instances, the mothers would wail louder, asking me not to leave until the baby is born. But sometimes labour can continue all night or all day. Everybody else gets scared in those circumstances, but not me.”
Often, she would ask for a little oil (any oil available in the kitchen) to massage the pregnant woman’s belly. Ropi says she can feel the belly and assess whether the child is in a breech position, or if the head of the foetus can be angled correctly with firm massaging in the right direction. She did come across instances of the child being born legs-first but claims she had no major trouble with these births too.
Other traditional beliefs have been tougher to shake off. If labour pains don’t begin after completion of the ninth month, Charku says she recommends a few sips of water blessed by a bhoomkal
The dai also usually cleans the birthing area after the delivery is completed, adds Ropi. “And earlier we used to bathe the child immediately. Now we’ve stopped doing that,” she says. The customary practice was to bathe the baby and only after that hand it over to the mother for the first breastfeeding.
Charku concurs. “Earlier, we would use warm water and bathe the baby immediately after birth. And sometimes the baby would be given mother’s milk only a couple of days later.” Some families gave the baby only jaggery-water or honey-water on the first day.
The practice of bathing the newborn is now rarely followed mainly due to advice from local ANMs, campaigns to promote institutionalised delivery and state-level attention to Melghat’s problem of infant mortality. (Various studies and reports have spoken of the region’s high infant mortality rate and severe malnutrition). The baby’s health is now usually prioritised over post-birth rituals and offerings to deities, says Bortyakheda’s ANM Shanta, and the government-UNICEF training helped ensure better safety levels in home birthing procedures.
Now, when the baby begins to stir after the mother has had a few minutes of rest, the dais show her how to breastfeed in a safe position while lying down or seated. And now the baby is given mother’s milk within half-an-hour, says Charku.
Other traditional beliefs have been tougher to shake off. If labour pains don’t begin after completion of the ninth month, Charku says she recommends a few sips of water blessed by a bhoomkal (a traditional spiritual healer).
Ropi says she likes to predict whether a pregnant woman will have a son or a daughter. Male foetuses, she claims, tend to give the belly a prominent protrusion. “Female foetuses make the belly appear spread-out around the sides.” But she also laughs off the generalisation, saying it’s a little bit of guesswork and that God never meant for humans to know the gender of a baby until it is born.
Left: Charku’s eyesight is dimming, and she tells families more and more frequently to head to the PHC or the new sub-centre. Right: Ropi too sends away most people who come to seek her help, telling them, ‘I can’t do it any longer’
In Bortyakheda, the villagers point out, traditional dais perform a supportive role in community health, improving last-mile delivery of state aid for pregnant women (including regular check-ups, supply of iron-folic acid and calcium supplements), planning for the birth and ensuring timely hospitalisation.
Villagers in Jaitadehi, much closer to Paratwada town’s private practitioners, are less concerned that they will not have a dai after Ropi. Meanwhile, Ropi says she may have a few things to tell government institutions where babies are delivered. “Some women are so thin, vomiting every day right through nine months. They refuse to eat meat, they make a face at some kinds of food. Pregnant women should eat everything. Nothing is forbidden,” she says. “Doctors should advise pregnant women on these things also.”
In her community, the dai is invited for the fifth-day celebrations after a baby is born to a Korku family. Often, she gets paid that day, a symbol that the baby has survived the early uncertain span. “Some die of accidents, some due to illness, some die in birth,” Ropi says, philosophically. “Everybody will die someday. But surviving childbirth is a victory for the mother and the child.”
The gratitude she received for the survival of babies was one of her biggest joys as a dai, Ropi says, and she misses this the most now that she is not so active. She sends away most people who come to seek her help: “ Jao baba, ab mere se hota nahi,” she tells them. “I can’t do it any longer.”
PARI and CounterMedia Trust’s nationwide reporting project on adolescent girls and young women in rural India is part of a Population Foundation of India-supported initiative to explore the situation of these vital yet marginalised groups, through the voices and lived experience of ordinary people.
Want to republish this article? Please write to zahra@ruralindiaonline.org with a cc to namita@ruralindiaonline.org








